As I have discussed previously in the pages of Developing Devotion, I was diagnosed with stage IV EGFR+ non-small cell lung cancer with metastases to the brain and spine in August 2023 . My treatment for this disease has included radiation to the brain and a wonder drug called osimertinib (aka Tagrisso) that targets and inhibits cells with the non-heriditary genetic mutation that most likely caused my cancer. (I’ve never smoked.) Fortunately, this course of treatment has been highly effective, resulting in significantly improved scans and symptoms.
Unfortunately, my affliction has recently reared its menacing head again.
The initial presentation of the cancer consisted of recurring visual auras (aka silent migraines) that eventually climaxed in a seizure on July 31 of last year. Thanks to my treatment, I have been blessedly free of seizures since that day (and visual auras since shortly after) until about a month ago. On May 31, I was in California where I had just attended my niece’s wedding and was working remotely at my sister’s house in Simi Valley when I was struck by my first visual aura in many months. My sister was able to transport me to an emergency department where I managed to make it onto a hospital gurney before my convulsions began.
Following my recovery and discharge, I was put on an anti-seizure medication called levetiracetam (aka Keppra) as well as a steroid called dexamethasone (aka Decadron) for the inflammation in the brain that most certainly caused my visual aura and seizure.
I was relieved to learn that subsequent brain scans indicate no worsening of the cancer. My oncology team believes that the episode was triggered by inflammation, which was caused by edema (a form of swelling) in my brain, which recently flared up due to brain tissue necrosis, which is a medium-term post-treatment effect of the radiation to my brain (and actually a long-term positive sign, since it means the cancer in my brain has been dying). It may seem like an oddly delayed reaction, but I am told that I am squarely in the post-radiation window of time within which this typically occurs for patients.
However, while the findings are cautiously optimistic for the long term, my situation is highly precarious in the short term. Until my immune system clears out the dead tissue and my brain swelling reduces, I’m still at a high risk for further seizures, which can lead to neurological damage and dangerous falls.
Moreover, the treatment I have received for this condition has proven nearly as debilitating as the condition itself, as the steroid I have been taking has given me a progressively worsening case of insomnia. My sleep has been decimated down to mere minutes a night, often making it hard for me to function or even think straight (although it has at times also led to bizarrely prolific bursts of adrenaline-fueled inspired lucidity).
My insomnia became so severe during a high-stakes work conference the other week that, out of desperation, I precipitously tapered myself off the steroid. My sleep has very slowly improved since then, but the insomnia has dragged on, in part because of harsh steroid withdrawal symptoms. And my calculus was further complicated by yet another visual aura and emergency department visit three days ago. The episode resulted in a brief loss of the right side of my field of vision, but thankfully did not climax into full-blown convulsions this time. This was perhaps owing to rapid intervention thanks to my wife having happened to drive by the Northeast Georgia Medical Center in Lumpkin shortly before the aura occurred on our way back from a one-night family getaway in a cabin in the woods. A young brown bear had recently bounded across the winding mountain road in front of us on our way to the highway, which may have been a sign of the peril to come.
My oncology team does not want me to taper off the steroid until after my MRI scheduled for early August, and only then if my brain edema shows improvement. Unfortunately, that is untenable for me, (1) because my body will suffer a system-wide collapse if my sleep does not improve, (2) because nothing I’ve tried (including melotonin) has been able to counteract the hyper-stimulating effects of the steroid, and (3) because I’ve tried nearly everything I’m willing to try. Going further down the side-effect spiral of pharmaceutical interventionism with a powerful drug like Ambien is a non-starter for me. So I have made the difficult decision to stay off the steroid to prevent reversing the precious progress I’ve made against the insomnia and to avoid having to go through withdrawals again.
Natural melatonin supplements have been a little helpful in restoring my sleep schedule as the steroids leave my body. But what has been most efficacious has been work I’ve done on what specialicsts call sleep hygiene, especially the sleep protocol I began iteratively developing during sleepless nights in my conference hotel room the other week.
My sleep protocol involves mnemonic tricks that prompt me to run iPhone automations, which in turn open Notion checklist that guide me through specific contingency plans for bouts of both sleepiness and wakefulness. The protocol simplifies my decisions about when to get busy sleeping and when to get busy rising and has helped me form reliable habits that cue sleep like clockwork.
The protocol also involves tracking my sleep, both with my Apple Watch and by logging my bedtimes and waking times on my iPhone. What you measure, you manage, so keeping score of my sleep has helped me to improve upon it.
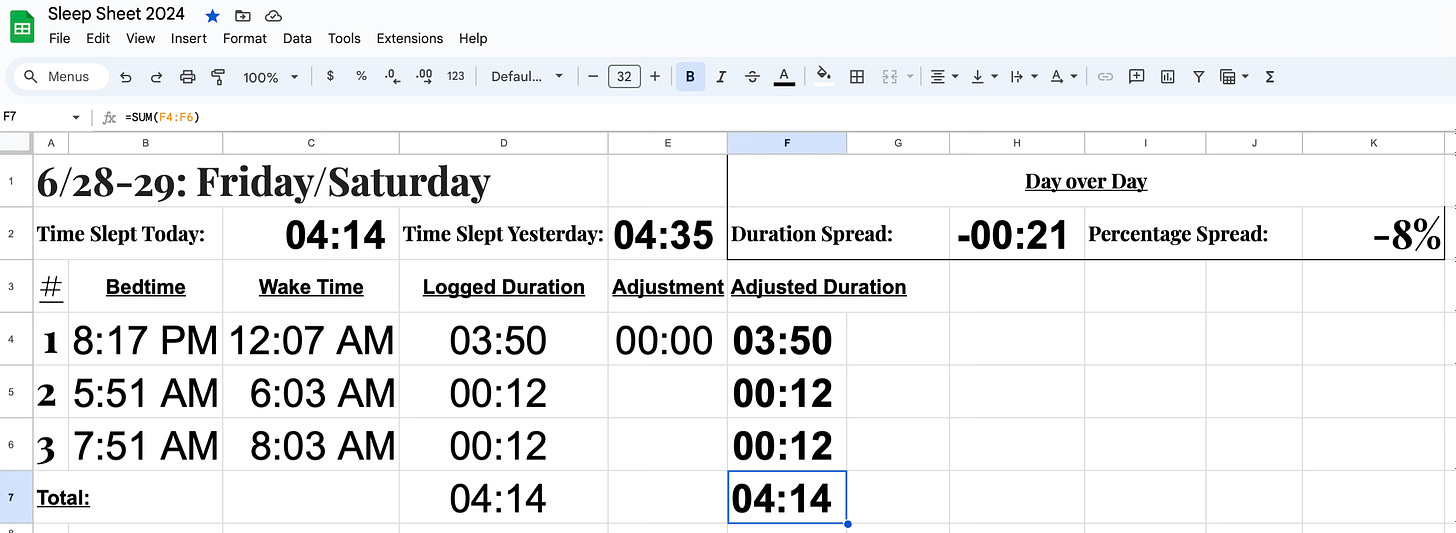
Whenever I bed down or wake up, I tap a button on my phone that logs the time. Later, I plug those times into a spreadsheet I designed for sleep analysis, which I use to tally up my minutes spent asleep. My daily score starts at my nightly bedtime. My night’s sleep lays an initial foundation, which I then build on with naps throughout the day to try to beat my score from the previous day. Here’s a screenshot of today’s tab in my “Sleep Sheet”:
Four-plus hours of sleep is still not enough, but it is a massive improvement for me, especially given that only a few nights ago I only managed 15 minutes. Blue-light screen time is generally thought to be antithetical to good sleep. But used briefly and judiciously, it can be a clutch sleep hygiene practice.
As calmly rational as I currently am about all this, it has been quite an ordeal. But the way to get through any health struggle is to take on the role, not of a mere victim and patient, but that of an agent and one’s own chief care provider. And, my experience and observations have convinced me that, by and large, the best form of care consists, not of an endless chemical barrage of patented pills, but of healthy lifestyle choices, practices, and behaviors.
I choose to treat this ordeal as a gauntlet, because gauntlets can make you spiritually stronger which is the surest path to becoming physically healthier.
Thank you for reading. If you would like to help my family with our mounting medical expenses, we are still accepting donations through GiveSendGo.